Impact: Improving the lives of military veterans with Post Traumatic Stress Disorder
-
Tagged under
Health and wellbeing
-
Lead Academics
Dr Mark Wheeler
Professor Sheina Orbell
Dr Nick Cooper
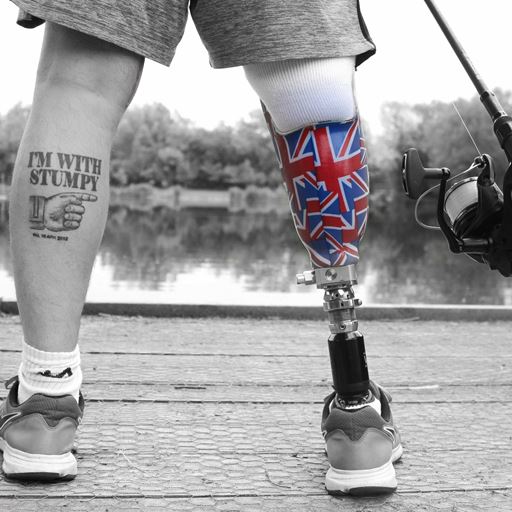
A programme, developed at Essex, is improving the lives of military veterans by helping them overcome the debilitating symptoms of Post Traumatic Stress Disorder (PTSD).
Over 100 veterans have benefitted so far, with participants reporting reduced symptoms and an improvement both in their ability to work and in their personal lives.
Post Traumatic Stress Disorder
PTSD is the psychological distress suffered by someone following a traumatic event, such as a serious accident, bereavement or military combat.
Most people overcome the effects of such an event without professional help, but those who develop PTSD can experience nightmares, intense anxiety and difficulty communicating. It can dramatically reduce their quality of life - impacting on both their ability to work and on their personal relationships.
As a psychological therapist working in the NHS, Dr Mark Wheeler realised the patients he was seeing from Colchester Garrison were just the tip of the iceberg. Many more needed help, but a new approach was needed for those reluctant to engage with traditional therapy.
While continuing with his clinical work, Mark embarked on a PhD, supervised by Professor Sheina Orbell from the Department of Psychology, to find a way of helping more veterans.
What we did
Alternative approaches have been tried elsewhere – a programme in America took veterans canoeing, while a UK study tried surfing. Although these proved popular, there has been no measure of how successful they were.
Mark drew on psychological theory and research from our Green Exercise Team, which has shown the enormous benefits to health and wellbeing of being outside, to develop a new support programme.
It comprises three elements – green exercise (particularly fishing) encouragement for veterans to share their experiences, rather than bottling up their feelings, and on-going peer support.
What changed
The results have been remarkable. Scientific analysis has shown the psychological wellbeing of participants has improved and the veterans themselves have reported a dramatic reduction in their symptoms which has set them on the road to recovery.
“We interviewed participants three years after the original intervention. One, who was unemployed because of the severity of his symptoms has started an Open University degree, got engaged and become a father again, while others have returned to full-time work, got married or re-established broken relationships.”
The success of the programme has been recognised by the NHS, the armed forces and charities, including Veterans First, Combat Stress and the Invicta Foundation, who continue to refer clients to Mark for help.
Major Stuart Lennox, of the Royal Air Force, joined a fishing trip to France which included veterans from Afghanistan, Iraq, Northern Ireland and the Gulf War. He said: “The visible benefits of the study were clear to see in every single participant. The programme is unique and is head and shoulders above the rest in the level of support it offers, the academic research that underpins its output and the professional manner with which it is delivered.”
Mark has finished his PhD and returned to full-time clinical work, but his support for veterans continues. Together with Dr Nick Cooper, from the Department of Psychology, he set up a not-for-profit company, iCARP, to organise more trips for veterans and emergency services staff.


